Whether you have a recent diagnosis or you have had diabetes for years, it’s important to be aware of diabetic retinopathy. Diabetic retinopathy is a complication that can develop in anyone with diabetes.
You can protect the quality of your vision by knowing about the signs, diagnostic tests, available treatments, and means of preventing the condition from developing in the first place. Keep reading to learn more about diabetic retinopathy, including how you can know if you might have it!
What is Diabetic Retinopathy?
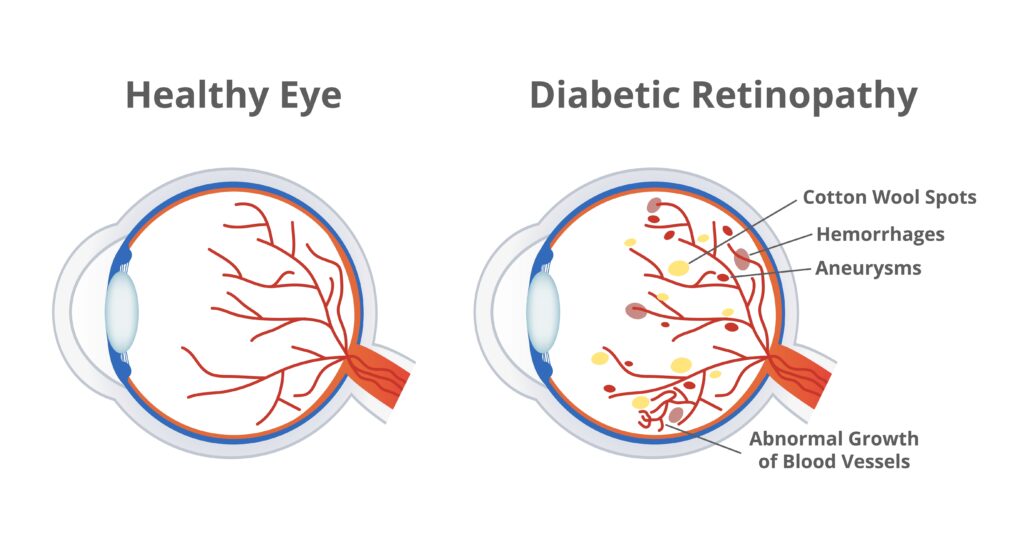
Diabetic retinopathy happens when the blood vessels in the retina, the light-sensitive tissue at the back of the eye, are damaged by elevated blood sugar levels. High blood sugar levels decrease the elasticity of blood vessels, causing them to narrow and impede regular blood flood.
Over time, diabetic retinopathy can cause the damaged blood vessels to swell and leak. It can also result in the growth of abnormal blood vessels.

There are two main types of diabetic retinopathy:
Non-Proliferative Diabetic Retinopathy (NPDR)
NRDR is the early stage of diabetic retinopathy. It is characterized by weakened blood vessels that leak fluid and blood into the vitreous, causing swelling and reducing oxygen supply to the retina.
Proliferative Diabetic Retinopathy (PDR)
PDR is the more advanced stage of diabetic retinopathy. At the PDR stage, the retina develops new, abnormal blood vessels, which can bleed into the eye and lead to scar tissue formation.
PDR can cause severe vision impairment or blindness if not treated promptly. If left untreated, diabetic retinopathy can lead to more serious eye conditions, including macular edema, glaucoma, and retinal detachment.
These conditions can lead to severe vision impairment, including blindness.
What are the Signs of Diabetic Retinopathy?

Diabetic retinopathy develops slowly, and it may take years for signs of the condition to become noticeable. As the condition progresses, some of the most common signs include:
- Blurred vision
- Fluctuations in vision clarity
- Floaters or spots in the field of vision
- Dark or empty areas in the vision
- Impaired color vision
- Difficulty perceiving contrast
When diabetic retinopathy has reached the PDR stage, a person with it may also experience tunnel vision, significant but temporary visual impairment, or the complete and permanent loss of central vision.
What are the Tests for Diabetic Retinopathy?
Because diabetic retinopathy can be asymptomatic until significant damage has occurred, it is important for individuals with diabetes to schedule bi-annual or annual comprehensive eye exams.
During these eye exams, an eye doctor often performs the following tests to check for signs of diabetic retinopathy:

Visual Acuity Test
This test assesses the clarity of one’s vision using a standardized eye chart.
Dilated Eye Examination
After dilating the pupils with special eye drops, this test enables the eye doctor to get a detailed examination of the retina and other structures within the eye.
Fundus Photography
Fundus photography, which is used to capture a detailed image of the retina, can document changes to the retina over time, leading to early diagnosis and effective treatment planning.
Optical Coherence Tomography (OCT)
This advanced imaging technology produces cross-sectional images of the retina to detect any swelling or thinning of retinal layers more accurately.
All of these tests are done right in an eye doctor’s office. These are minimally invasive and quick.
How is Diabetic Retinopathy Treated?
Because the damage to the retina caused by diabetic retinopathy is often irreversible, the main objective of treatment is the prevention of further damage to the structures of the eye.
When diagnosed at the NDPR stage, the recommended treatment may be more careful monitoring of blood sugar levels. Effective management of blood sugar may help prevent or slow the progression of diabetic retinopathy.
If diabetic retinopathy has progressed further and is starting to affect a person’s vision, the following treatments may be suggested:
Retinal Injections
In this treatment, medications that can reduce swelling, leakage, and abnormal blood vessel growth are administered directly into the eye.
Laser surgery
Laser surgery, or pan-retinal photocoagulation (PRP), can help seal leaking blood vessels and prevent further damage to the retina and other structures within the eye.
Vitrectomy
The most advanced cases of diabetic retinopathy, where excessive bleeding or retinal detachment has occurred, may require the surgical removal of the vitreous gel from the eye.
Is Diabetic Retinopathy Preventable?
If you have diabetes, there are steps you can take to help prevent diabetic retinopathy. These steps include:
- Carefully managing blood sugar levels with medication and lifestyle modifications
- Monitoring and controlling both blood pressure and cholesterol levels
- Quitting or avoiding smoking as well as excessive alcohol consumption
- Adopting a healthy diet and regular exercise routine
- Scheduling regular comprehensive eye exams
Having diabetes does not mean inevitable vision impairment from diabetic retinopathy. By knowing what signs to look for, taking preventive steps, and scheduling regular eye exams, you can ensure that your clear eyesight is protected from this common diabetes complication.
Do you have diabetes and notice signs of diabetic retinopathy? Schedule an appointment at Nevada Eye Physicians in Las Vegas, NV, today!



